Understanding Plantar Fasciitis
About Plantar Fasciitis
Plantar fasciitis physiotherapy helps relieve heel pain, restore mobility, and address the underlying causes of plantar fascia strain. At Rehab8, our goal is not only to reduce symptoms but to provide targeted plantar fasciitis treatment that improves foot mechanics and prevents future flare-ups.At Rehab8, our personalized plantar fasciitis therapy focuses on relieving pain, improving foot and ankle mobility, and strengthening the structures that support healthy movement.
What Is Plantar Fasciitis and What Causes It?
The plantar fascia is a thick connective tissue that runs from the heel bone to the toes, supporting the arch of the foot and helping absorb impact during movement.
When excessive strain is placed on this tissue, small micro-tears can develop. This leads to inflammation, stiffness, and heel pain - especially after periods of rest.
Many people with plantar fasciitis notice symptoms such as:
- Sharp heel pain with the first steps in the morning
- Pain after long periods of sitting or inactivity
- Tenderness along the heel or arch
- Stiffness in the foot or ankle
- Pain that increases after prolonged standing or activity
Early plantar fasciitis physiotherapy can significantly reduce recovery time and prevent the condition from becoming chronic.
Plantar fasciitis typically develops due to repetitive stress rather than a single injury. Several factors may increase strain on the plantar fascia.
Common Causes and Symptoms
Plantar fasciitis typically develops from repeated strain on the plantar fascia, rather than a single injury. It can affect people who are on their feet for long periods, runners, or those with poor foot mechanics.
- Overuse or Repetitive Stress: Activities that involve running, jumping, or prolonged standing can strain the plantar fascia.
- Foot Mechanics: Flat feet, high arches, or abnormal walking patterns can place uneven pressure on the heel and arch.
- Improper Footwear: Shoes with poor arch support or thin soles can contribute to irritation.
- Tight Calf Muscles or Achilles Tendon: Limited ankle mobility increases strain on the plantar fascia.
- Sudden Increase in Activity: Rapid changes in exercise intensity or duration can lead to inflammation.
- Excess Weight: Added body weight increases stress on the feet, especially the heels.
Identifying these factors is an important part of effective plantar fasciitis treatment.
Common Symptoms
- Sharp heel pain with the first few steps in the morning
- Pain after long periods of sitting or rest
- Tenderness or aching in the heel or arch of the foot
- Stiffness in the ankle or foot after standing for long periods
- Pain that increases after activity, rather than during it
Early recognition and treatment are important to prevent chronic discomfort or compensatory pain in the knees, hips, or lower back.
How Physiotherapy Helps Recovery
Professional plantar fasciitis physiotherapy addresses both the symptoms and the underlying biomechanical causes of heel pain. At Rehab8, our treatment plans are tailored to each patient’s movement patterns and lifestyle.
Assessment and Diagnosis
Your physiotherapist will evaluate:
- Foot and ankle mobility
- Walking or running mechanics
- Muscle flexibility and strength
- Posture and weight distribution
- Footwear and activity habits
This helps identify the root cause of your symptoms and guides your plantar fasciitis therapy plan.
Pain Relief and Inflammation Reduction
Early treatment focuses on reducing irritation and supporting tissue healing.
Treatment may include:
- Manual therapy
- Soft tissue release
- Joint mobilization
- Therapeutic modalities such as ice or ultrasound
These techniques help decrease inflammation and relieve heel discomfort.
Stretching and Strengthening
Weak foot and lower-leg muscles can increase strain on the plantar fascia.Targeted strengthening exercises focus on:
- Intrinsic foot muscles
- Calf muscles
- Achilles tendon
- Foot and ankle mobility
These exercises improve arch support and help prevent recurring symptoms.
Gait and Posture Correction
Improper walking mechanics can overload the heel and plantar fascia.
Your physiotherapist may assess and correct:
- Walking patterns
- Running mechanics
- Weight distribution
- Postural alignment
Improving movement patterns is a key part of long-term plantar fasciitis treatment.
Footwear and Orthotic Guidance
Proper footwear plays an important role in recovery.
Your physiotherapist may recommend:
- Supportive shoes with adequate cushioning
- Temporary heel support
- Custom orthotics if necessary
These solutions help reduce strain during daily activities.
Education and Prevention
You’ll receive practical advice on activity modification, load management, and home exercises to help maintain mobility and reduce the risk of recurrence.
Benefits of Plantar Fasciitis Physiotherapy
Effective plantar fasciitis therapy can help you:
- Reduce heel and arch pain
- Improve foot and ankle mobility
- Restore normal walking mechanics
- Prevent recurring flare-ups
- Return to sports and daily activities safely
With a structured physiotherapy plan, many individuals experience significant improvement without invasive treatments.
When to Seek Plantar Fasciitis Treatment
You should consider professional care if you experience:
- Persistent heel pain lasting more than 1–2 weeks
- Pain that worsens after activity
- Difficulty walking comfortably
- Stiffness in the foot after rest
- Recurring episodes of heel pain
Physiotherapy treatment offers a holistic approach to addressing plantar fasciitis. Our team combines manual therapy, exercise programs, and foot care strategies to improve function and reduce discomfort. With plantar fasciitis therapy at Rehab8, you benefit from:
- Personalized care: Tailored to your symptoms and lifestyle
- Effective pain management: Reduces discomfort and inflammation
- Long-term support: Prevents future flare-ups through muscle strengthening, movement correction, and guidance on footwear
- Proven outcomes: Our physiotherapists use evidence-based techniques to ensure the most effective care for you
Early plantar fasciitis physiotherapy can help speed recovery and reduce the risk of chronic foot problems.
Our Physiotherapy Treatment Approach
Progress at Rehab8 follows a structured system. Our physiotherapy services assess how your body moves, identify the true source of dysfunction, and utilize an established framework to restore your control, strength, and long-term function.
1. Reset
Focus: Relieving pain and restoring baseline mobility
- Manual therapy and gentle mobilisations
- Pain and inflammation management
- Postural and movement assessment
- Identification of underlying dysfunction
2. Reactivate
Focus: Re-engaging muscles and restoring control
- Manual activation exercises
- Neuromuscular re-education
- Functional mobility drills
- Improved circulation and joint movement
3. Retrain
Focus: Strength, stability, and movement quality
- Individualized therapeutic exercise programs
- Movement pattern correction
- Balance and coordination training
- Activity-specific rehabilitation for work or sport
4. Reinforce
Focus: Long-term results and injury prevention
- Home exercise and self-management strategies
- Posture and ergonomic guidance
- Lifestyle and load-management education
- Ongoing monitoring and plan adjustments
This framework ensures your physiotherapy services deliver measurable and sustainable results.
Why
choose us?
Your first session is a chance for us to get to know your body, understand its strengths and weaknesses, and identify any areas that need attention.
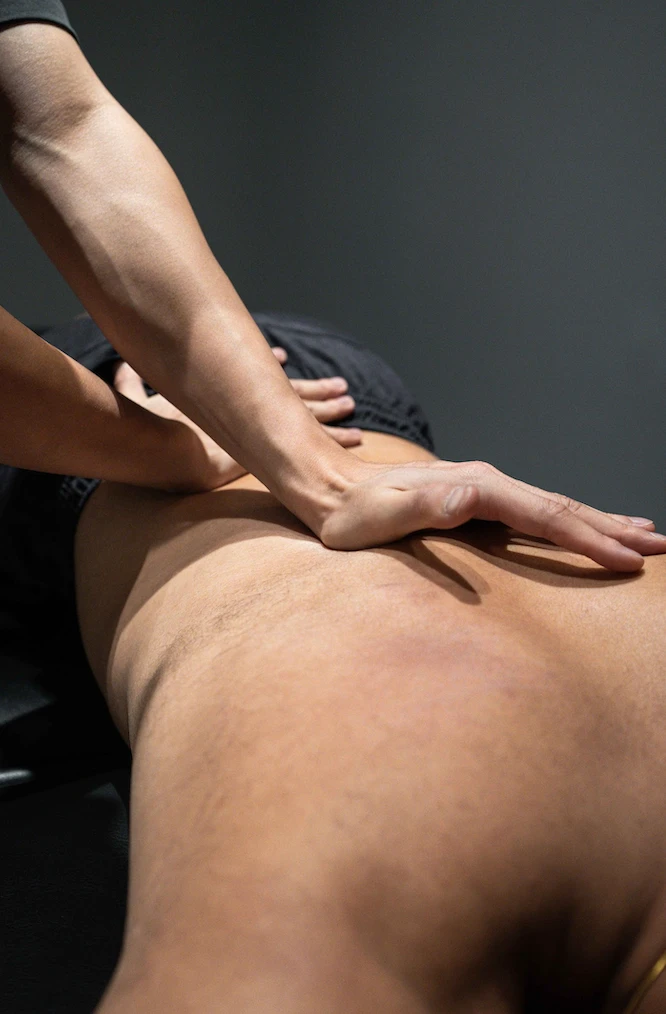
We design your session around your needs, goals, and lifestyle, combining manual therapy, modalities, and corrective exercises for optimal results.
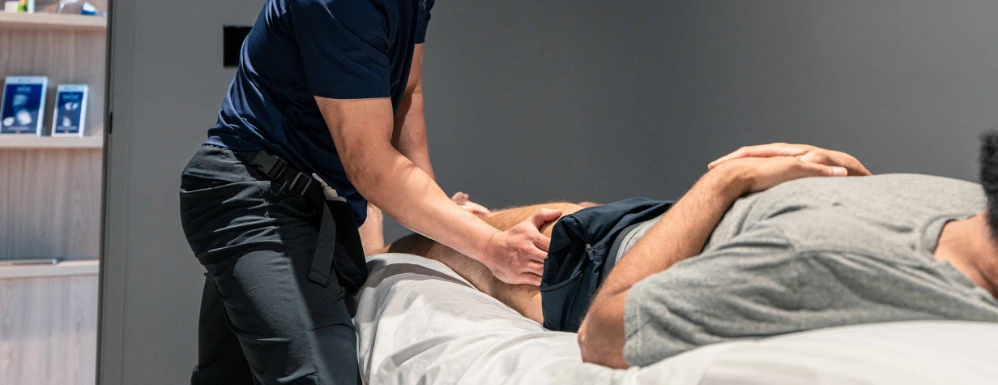
We take a whole-body approach to your wellbeing, helping you feel better, move more freely, and enjoy a healthier, more active, and balanced life.
Got a question for us?
Check below to see if we have an answer for you. If you can’t find the information you’re looking for, please contact us and we’ll be happy to help.
With consistent plantar fasciitis physiotherapy and proper care, most people experience improvement within 6 to 8 weeks. Chronic cases may take several months, depending on the severity of the condition and contributing factors such as foot mechanics and activity levels.
While high-impact activities should be reduced temporarily, gentle stretching and low-impact exercises are encouraged. Plantar fasciitis therapy guided by a physiotherapist can help maintain movement without putting undue strain on the foot. Strengthening exercises and foot mobility drills will also support recovery.
Yes. By improving foot strength, flexibility, and walking mechanics, physiotherapy for plantar fasciitis reduces strain on the plantar fascia and lowers the risk of future flare-ups. Targeted strengthening and proper movement patterns can help prevent the recurrence of this condition.
Get started
today.
We're excited to meet you and help you recover!
